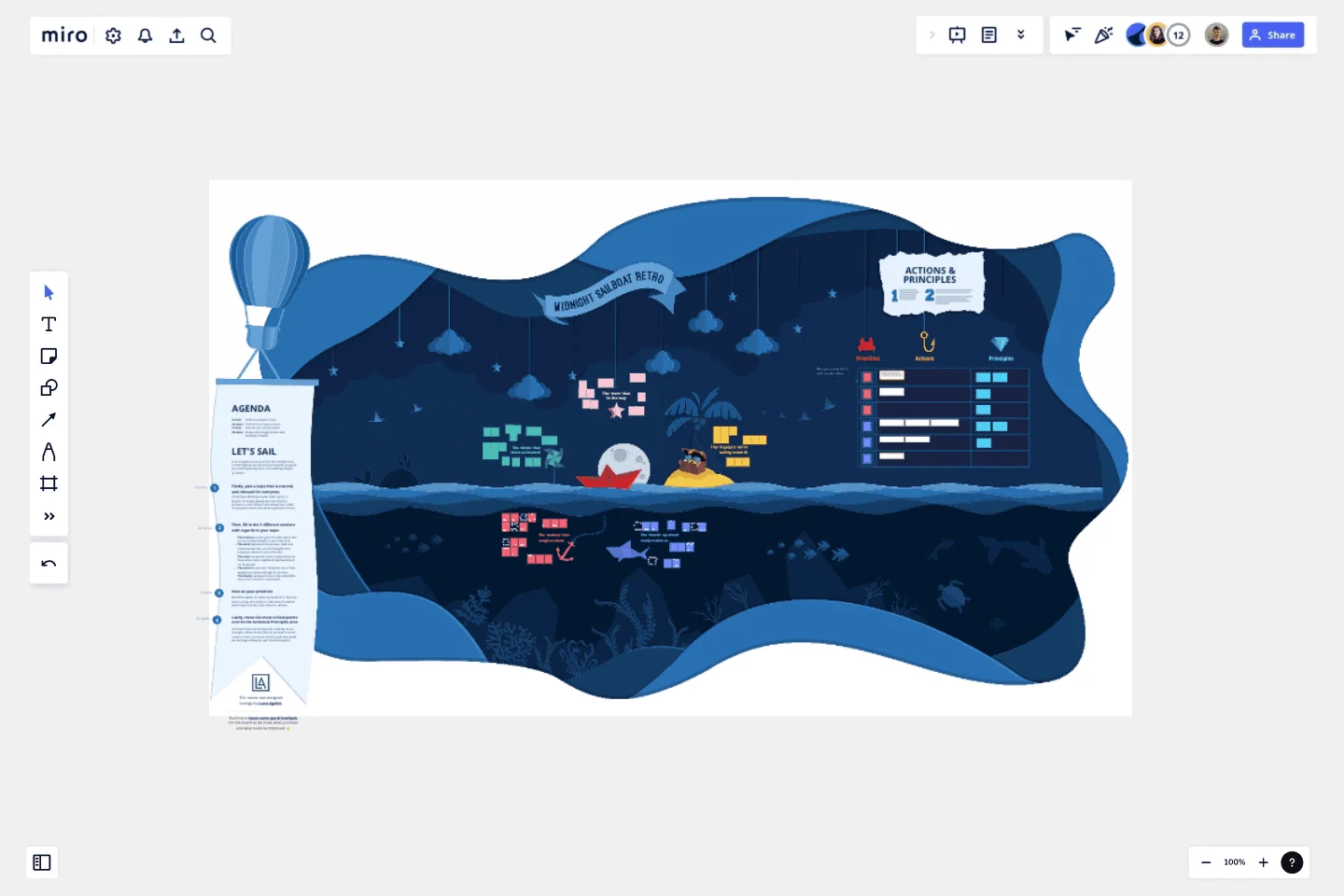
⚓️ Midnight Sailboat Retrospective
Sail toward action items with this fun template.
About
Transport your team to the delightful World of Papercraft, where we will sail the midnight seas together, and use our time riding tides to reflect on where we've done well and what we could improve for next time.
---
For who and for when?
This template is a perfect companion for teams who want to learn from recent sprints, projects, events or processes, and create actionable tasks and guiding principles to keep the future compass steady.
---
Why use this template?
This template is designed to take you on a visual experience that's easy to use, fun to explore, and most importantly it's actionable - so you can fully let go of your heaviest anchors and never meet the same sharks twice!
---
Credits
Cudos to the original creator of the Sailboat exercise, who devised a method so popular, it is impossible to identfy the first edition in amongst all the remakes. Good job! 🎉
Get started with this template right now.
Sailboat Template
Works best for:
Agile Methodology, Meetings, Retrospectives
The Sailboat Retrospective is a low-pressure way for teams to reflect on how they handled a project. By defining your risks (the rocks), delaying issues (anchors), helping teams (wind), and the goal (land), you’ll be able to work out what you’re doing well and what you need to improve on for the next sprint. Approaching team dynamics with a sailboat metaphor helps everyone describe where they want to go together by figuring out what slows them down and what helps them reach their future goals.
The Hot Air Balloon Retrospective
The Hot Air Balloon is a simple activity for helping the team identify things that makes them move faster, and things that slow them down.