October 14
Registration is live for Miro’s biggest event of the year — Canvas 25! Sign up now to secure your spot for October 14
REGISTER NOW
NYC or Virtual
Registration is live for Miro’s biggest event of the year — Canvas 25! Sign up now to secure your spot for October 14
REGISTER NOW
Registration is live for Miro’s biggest event of the year — Canvas 25! Sign up now to secure your spot for October 14
REGISTER NOW
Registration is live for Miro’s biggest event of the year — Canvas 25! Sign up now to secure your spot for October 14
REGISTER NOW
Limited Availability
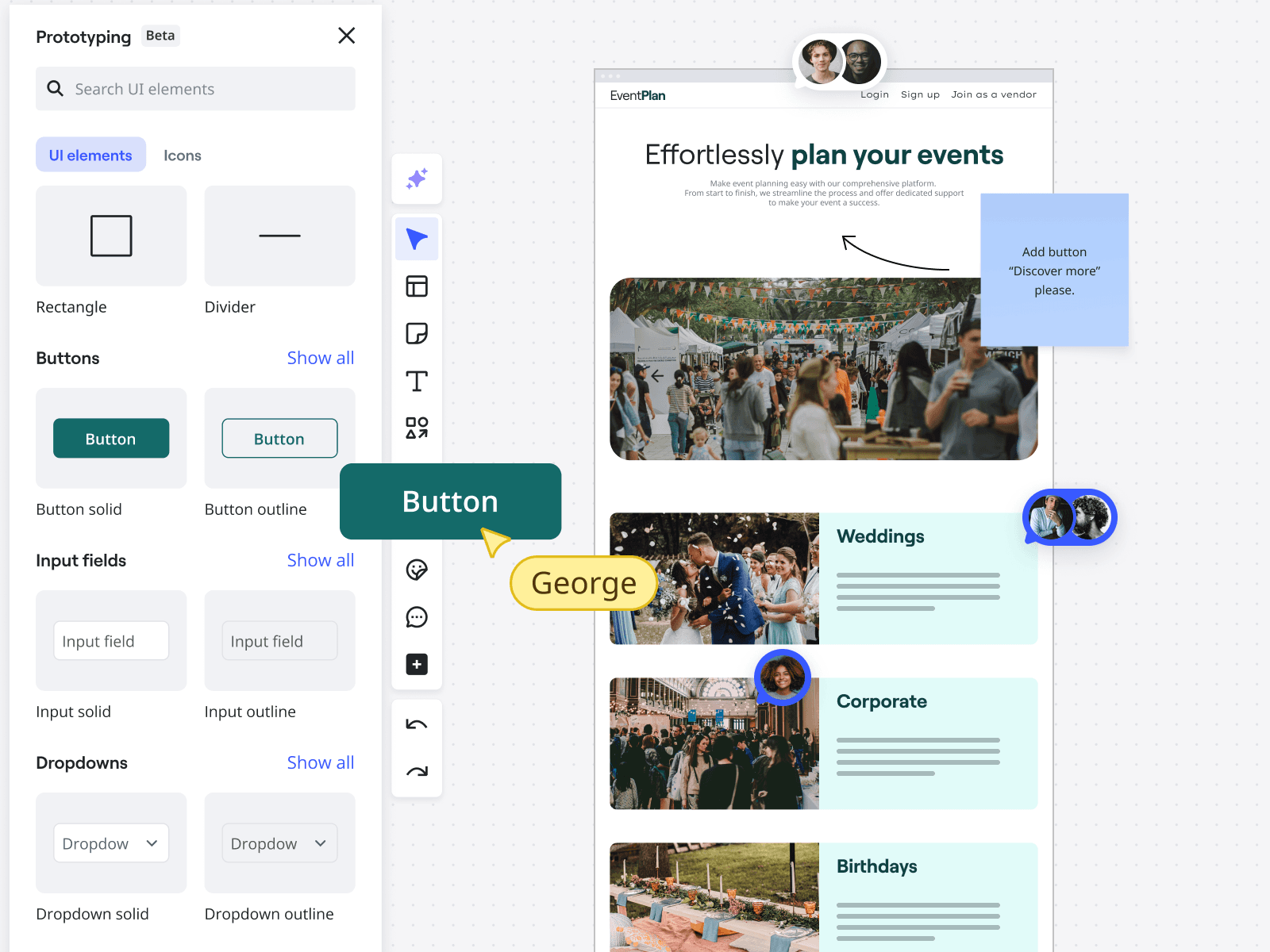
Collaborative AI prototyping
Turn messy ideas and structured research into professional, editable prototypes in minutes. Explore more directions, iterate faster, and align on better solutions before moving to design tools or code.
More than 90M users and 250,000 companies are collaborating in the Innovation Workspace
Why choose Miro for prototyping?
Explore more ideas and refine them easily
Align on direction to make quicker team decisions
Engage customers with visuals for faster buy-in
How it works
Turn what’s already on your canvas into prototypes in minutes. Miro Prototyping is built for fast, flexible collaboration—whether you’re exploring features or running a workshop.
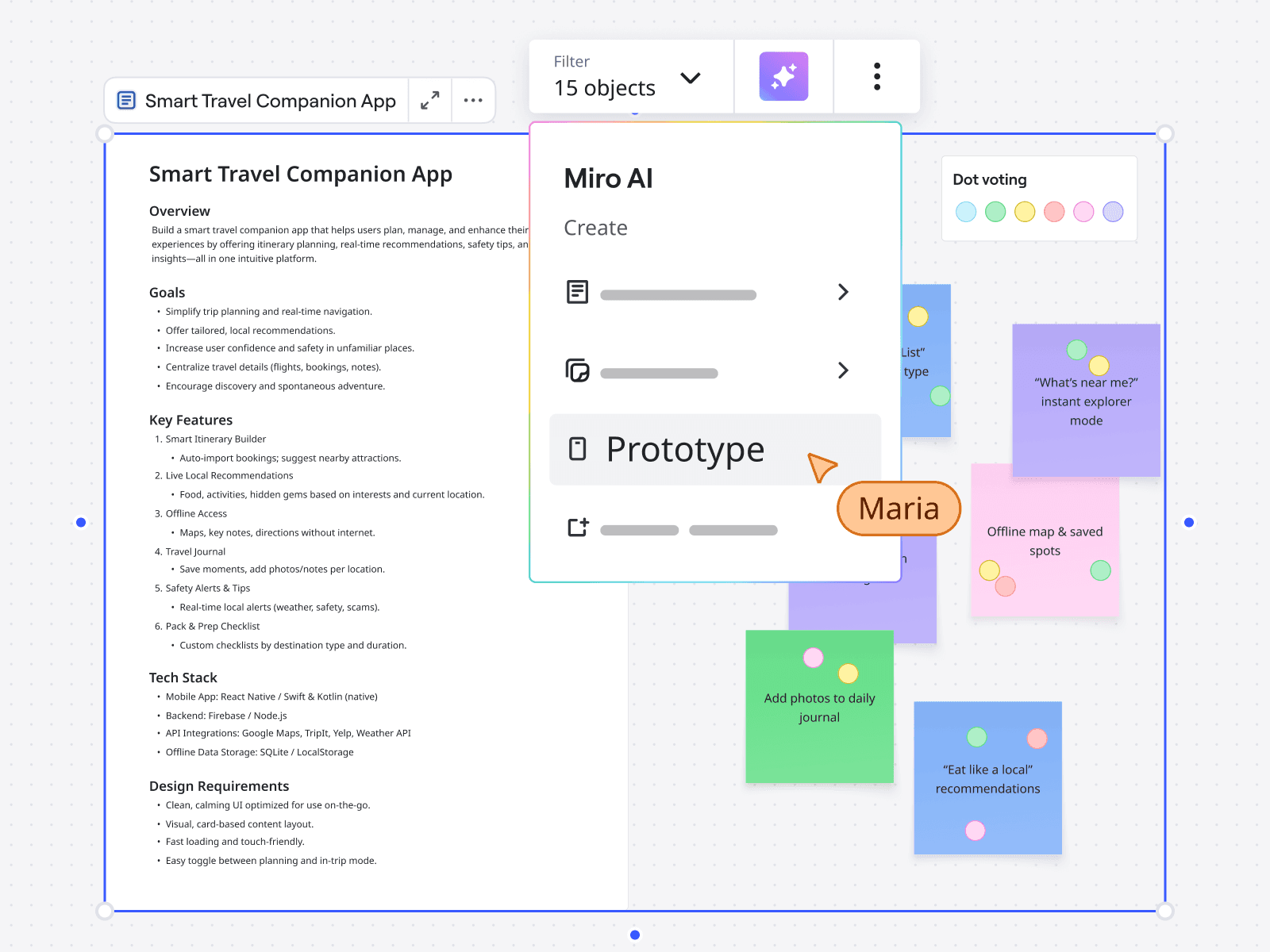
Create with AI
Generate multi-screen prototypes from sticky notes, screenshots, diagrams, or prompts using AI.
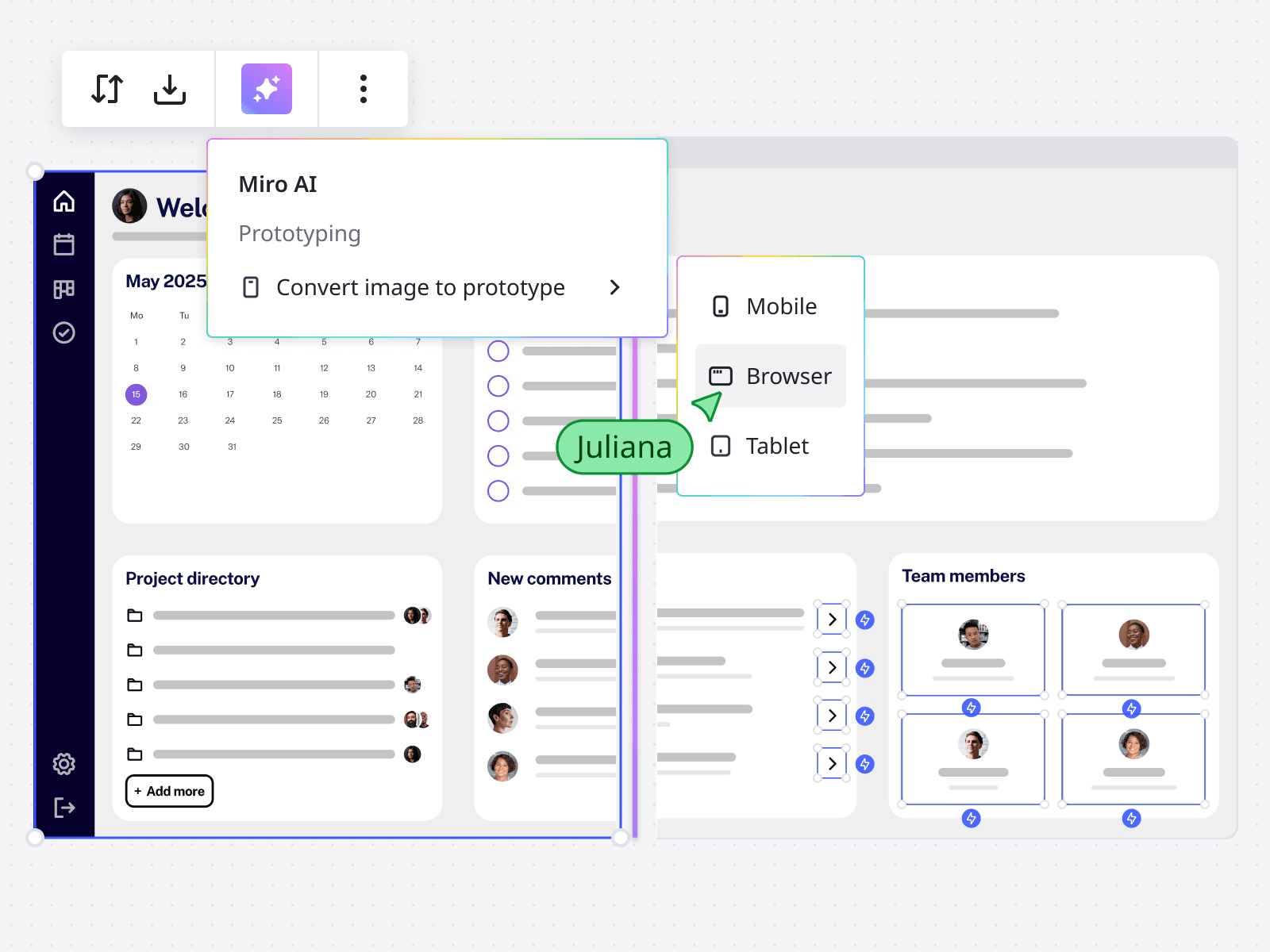
Start from a screenshot
Upload screenshots of apps or sites and turn them into mockups—no design files needed.
AI powered editing
Refine and remix with AI. Toggle between variations, tweak layouts, and land on the version that works best.

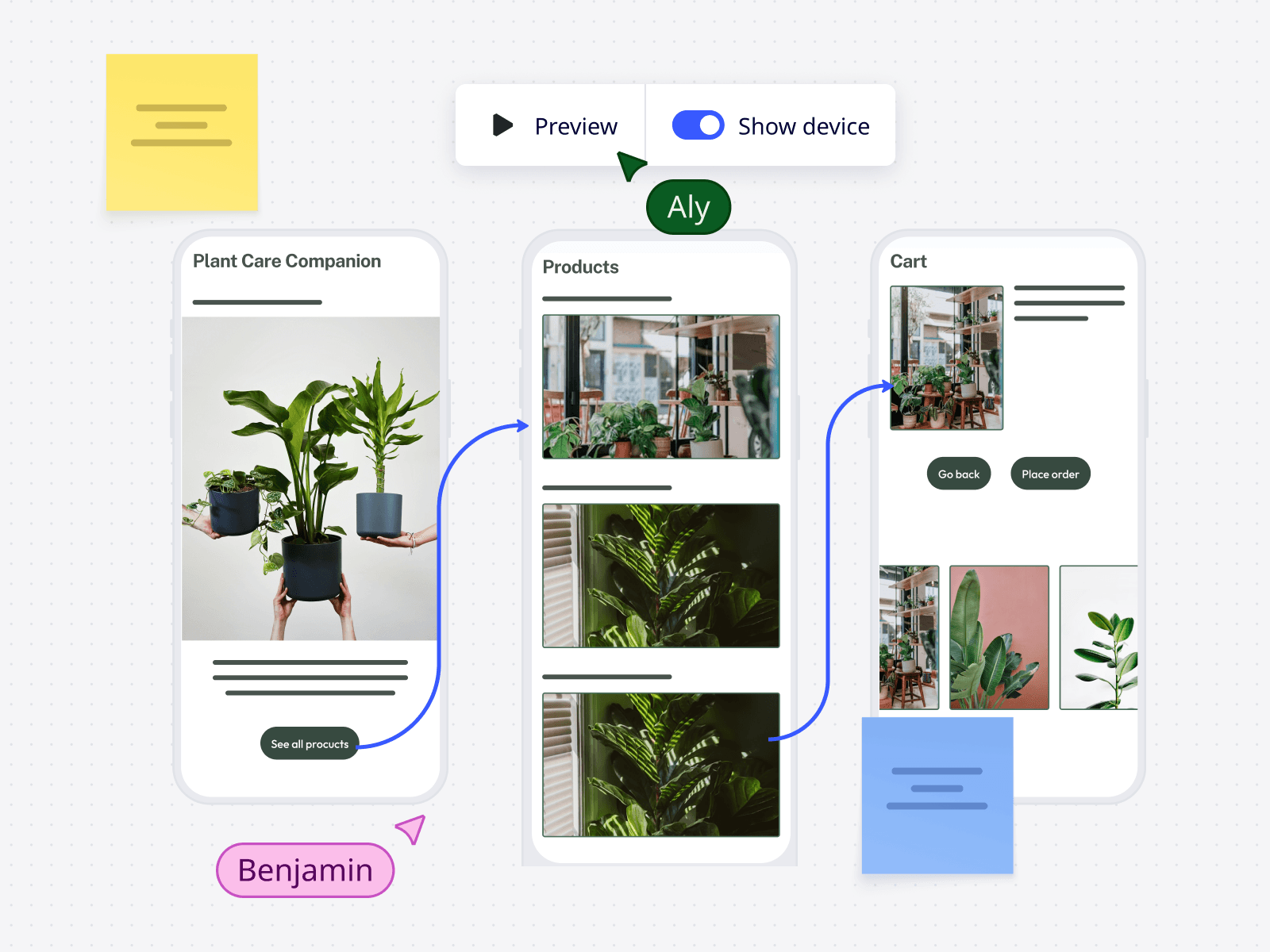
Preview and click through
Bring flows to life with clickable prototypes and guided hotspots—perfect for sharing, testing, and fast feedback.
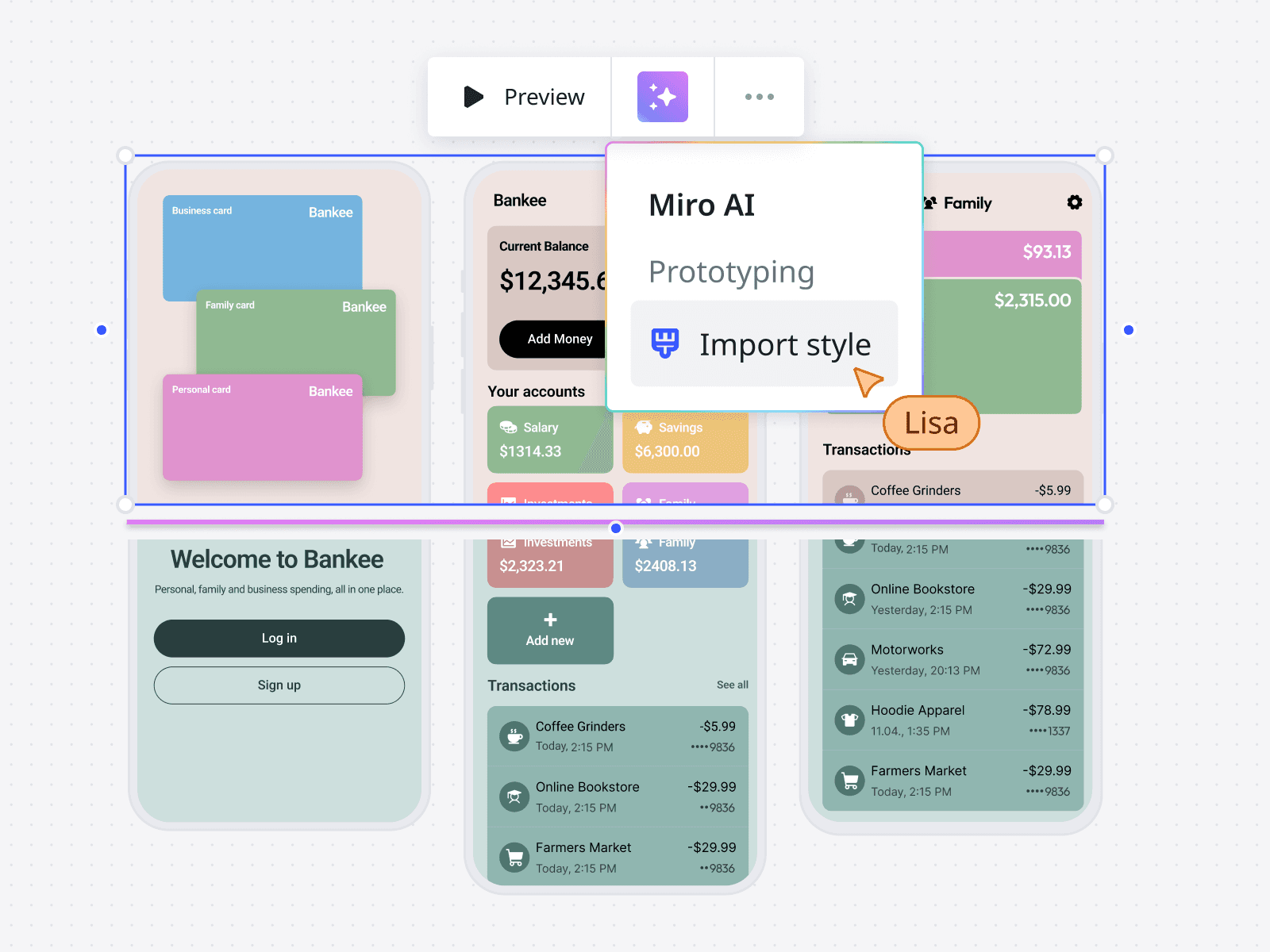
Style with brand assets
Upload a brand asset or screenshot to apply your colors—making prototypes feel more real with less effort.
Edit with drag-and-drop
Customize screens using editable components built for product flows.
Loved by product teams
Try the most popular templates tailored for your team
You’ll never need to start from scratch. Tap into Miro’s huge library of customizable templates, built for your everyday workflows.
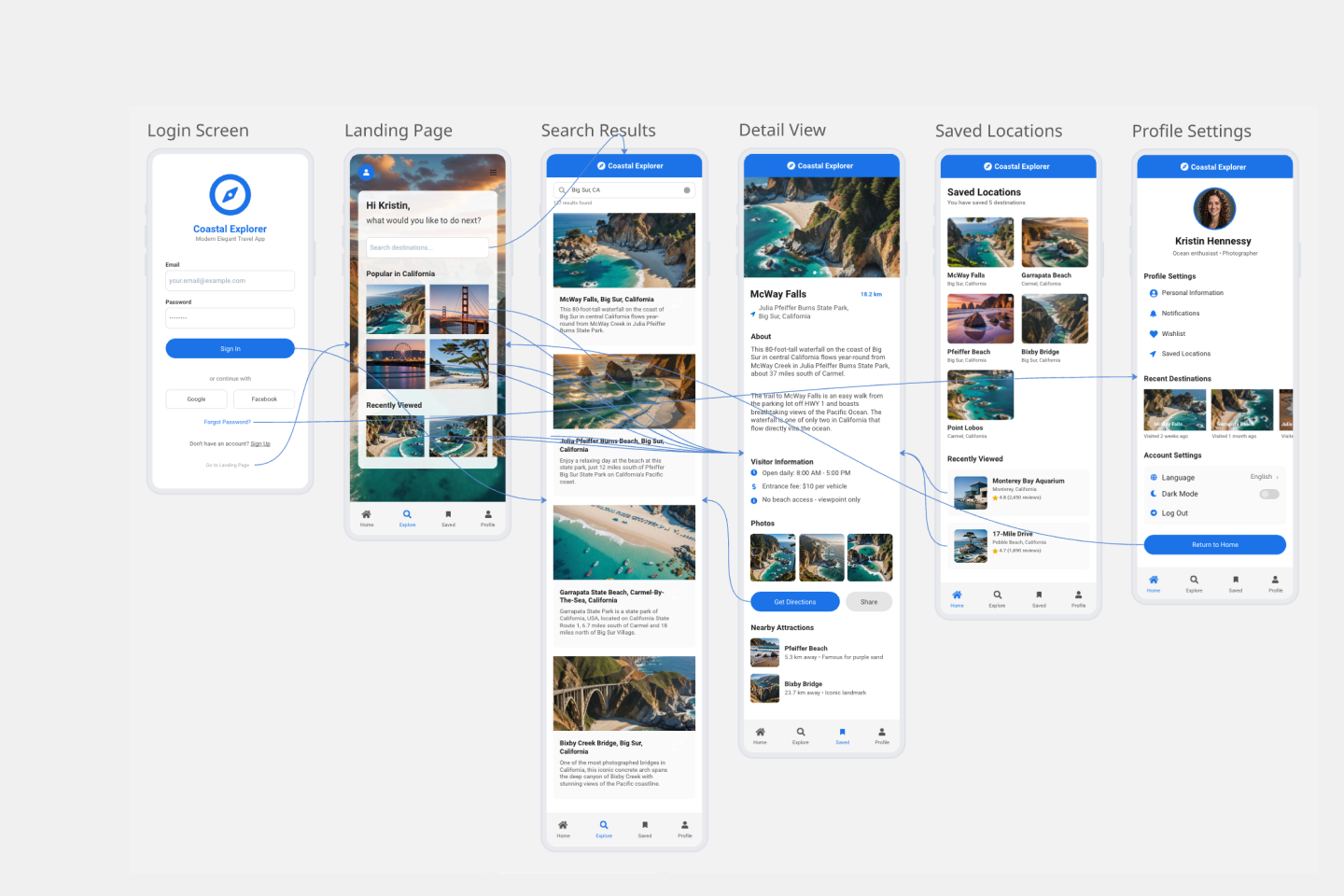
Create product prototypes, conduct usability testing, and gather stakeholder feedback.
21000b3c-2496-4e73-bc94-b59192206517
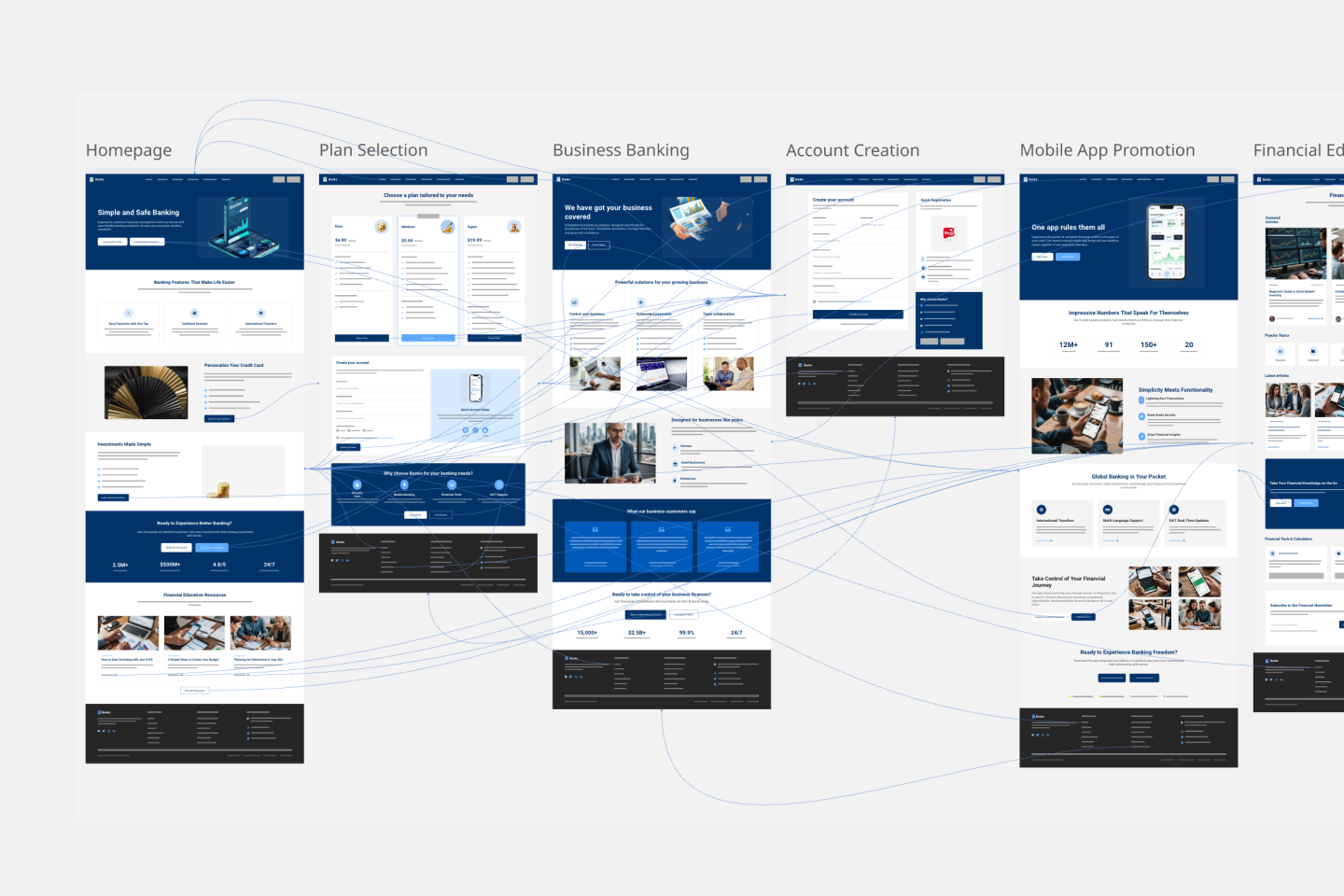
Visualize and iterate website designs using the latest AI capabilities for improved prototyping. Start off with our website prototype template.
95e82821-80c4-40d9-a78e-3c6eb1e720bc
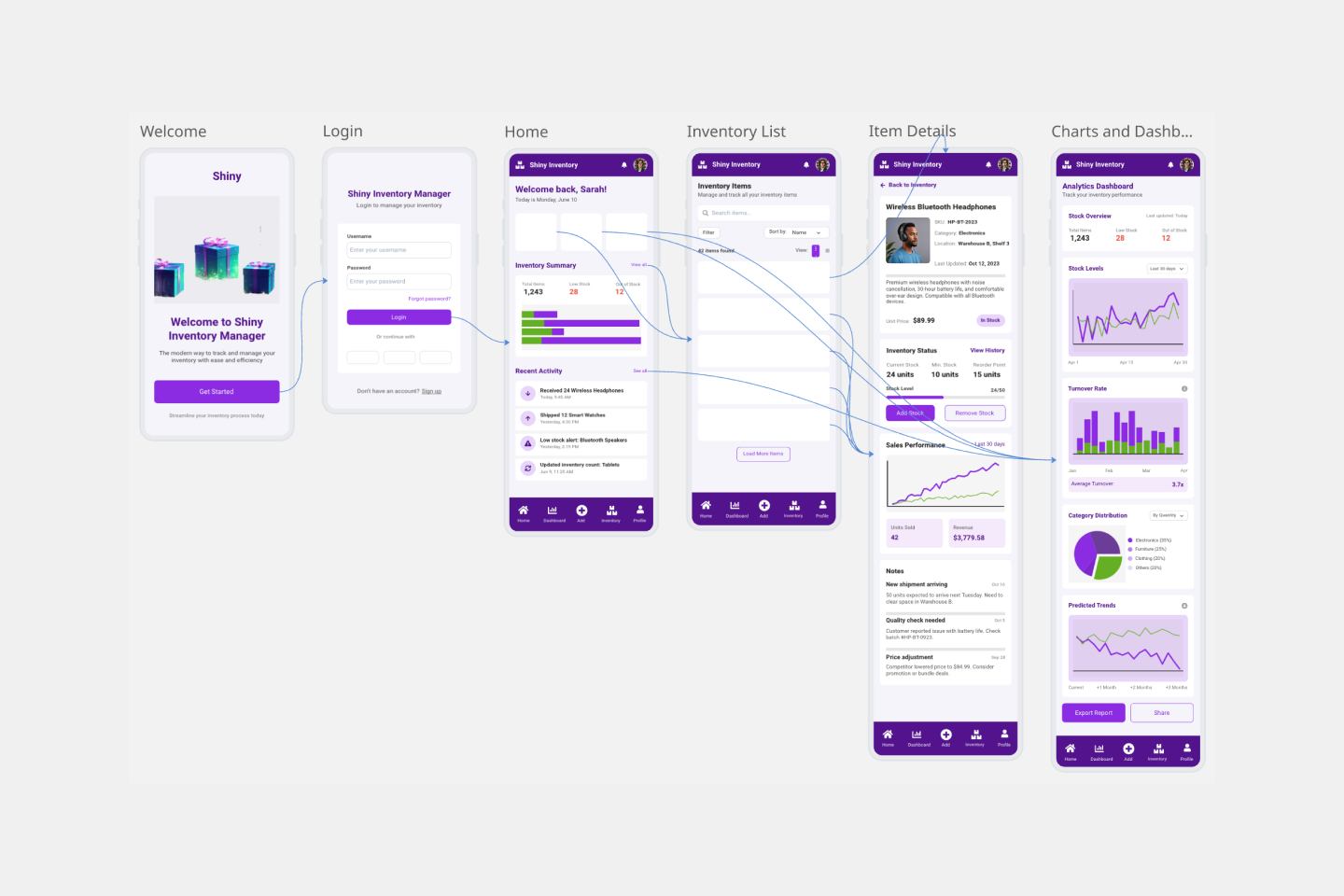
Streamline the creation and refinement of mobile app designs with the mobile app prototype template. Have a structured yet flexible framework that allows teams to quickly sketch, iterate, and perfect their app concepts.
78622b37-d691-4abd-a069-fbe4f3bade83
Map out your website elements, bring your vision to life, and create a better user experience.
bd2d2960-f2dd-4ca8-84a2-32d765faf126

Create the best version of your website or app prototype and get feedback early on.
3251bfb5-7a86-4987-aa30-75d35272caa8
Need help getting started?
Access free courses to ace the canvas in no time, browse through our blog, get quick answers from our Help Center, and more.
FAQs
What is Miro AI Prototyping?
Who is Miro Prototyping for?
What can I create with it?
How is this different from tools like Figma?
How is this different from vibe coding tools?
Can I use Miro Prototyping without enabling Miro AI?
Is my data used to train your AI models?
How does pricing work?
Is Miro Prototyping available for Enterprise plans?
Limited Availability
Collaborative AI prototyping
Turn messy ideas and structured research into professional, editable prototypes in minutes. Explore more directions, iterate faster, and align on better solutions before moving to design tools or code.
More than 90M users and 250,000 companies are collaborating in the Innovation Workspace
Why choose Miro for prototyping?
Explore more ideas and refine them easily
Align on direction to make quicker team decisions
Engage customers with visuals for faster buy-in
How it works
Turn what’s already on your canvas into prototypes in minutes. Miro Prototyping is built for fast, flexible collaboration—whether you’re exploring features or running a workshop.
Create with AI
Generate multi-screen prototypes from sticky notes, screenshots, diagrams, or prompts using AI.


Start from a screenshot
Upload screenshots of apps or sites and turn them into mockups—no design files needed.
AI powered editing
Refine and remix with AI. Toggle between variations, tweak layouts, and land on the version that works best.

Preview and click through
Bring flows to life with clickable prototypes and guided hotspots—perfect for sharing, testing, and fast feedback.

Style with brand assets
Upload a brand asset or screenshot to apply your colors—making prototypes feel more real with less effort.

Edit with drag-and-drop
Customize screens using editable components built for product flows.

Loved by product teams
Try the most popular templates tailored for your team
You’ll never need to start from scratch. Tap into Miro’s huge library of customizable templates, built for your everyday workflows.

Create product prototypes, conduct usability testing, and gather stakeholder feedback.
21000b3c-2496-4e73-bc94-b59192206517

Visualize and iterate website designs using the latest AI capabilities for improved prototyping. Start off with our website prototype template.
95e82821-80c4-40d9-a78e-3c6eb1e720bc

Streamline the creation and refinement of mobile app designs with the mobile app prototype template. Have a structured yet flexible framework that allows teams to quickly sketch, iterate, and perfect their app concepts.
78622b37-d691-4abd-a069-fbe4f3bade83

Map out your website elements, bring your vision to life, and create a better user experience.
bd2d2960-f2dd-4ca8-84a2-32d765faf126

Create the best version of your website or app prototype and get feedback early on.
3251bfb5-7a86-4987-aa30-75d35272caa8
Need help getting started?
Access free courses to ace the canvas in no time, browse through our blog, get quick answers from our Help Center, and more.
FAQs
What is Miro AI Prototyping?
Who is Miro Prototyping for?
What can I create with it?
How is this different from tools like Figma?
How is this different from vibe coding tools?
Can I use Miro Prototyping without enabling Miro AI?
Is my data used to train your AI models?
How does pricing work?
Is Miro Prototyping available for Enterprise plans?
Limited Availability
Collaborative AI prototyping
Turn messy ideas and structured research into professional, editable prototypes in minutes. Explore more directions, iterate faster, and align on better solutions before moving to design tools or code.
More than 90M users and 250,000 companies are collaborating in the Innovation Workspace
Why choose Miro for prototyping?
Explore more ideas and refine them easily
Align on direction to make quicker team decisions
Engage customers with visuals for faster buy-in
How it works
Turn what’s already on your canvas into prototypes in minutes. Miro Prototyping is built for fast, flexible collaboration—whether you’re exploring features or running a workshop.
Create with AI
Generate multi-screen prototypes from sticky notes, screenshots, diagrams, or prompts using AI.


Start from a screenshot
Upload screenshots of apps or sites and turn them into mockups—no design files needed.
AI powered editing
Refine and remix with AI. Toggle between variations, tweak layouts, and land on the version that works best.

Preview and click through
Bring flows to life with clickable prototypes and guided hotspots—perfect for sharing, testing, and fast feedback.

Style with brand assets
Upload a brand asset or screenshot to apply your colors—making prototypes feel more real with less effort.

Edit with drag-and-drop
Customize screens using editable components built for product flows.

Loved by product teams
Try the most popular templates tailored for your team
You’ll never need to start from scratch. Tap into Miro’s huge library of customizable templates, built for your everyday workflows.

Create product prototypes, conduct usability testing, and gather stakeholder feedback.
21000b3c-2496-4e73-bc94-b59192206517

Visualize and iterate website designs using the latest AI capabilities for improved prototyping. Start off with our website prototype template.
95e82821-80c4-40d9-a78e-3c6eb1e720bc

Streamline the creation and refinement of mobile app designs with the mobile app prototype template. Have a structured yet flexible framework that allows teams to quickly sketch, iterate, and perfect their app concepts.
78622b37-d691-4abd-a069-fbe4f3bade83

Map out your website elements, bring your vision to life, and create a better user experience.
bd2d2960-f2dd-4ca8-84a2-32d765faf126

Create the best version of your website or app prototype and get feedback early on.
3251bfb5-7a86-4987-aa30-75d35272caa8
Need help getting started?
Access free courses to ace the canvas in no time, browse through our blog, get quick answers from our Help Center, and more.
FAQs
What is Miro AI Prototyping?
Who is Miro Prototyping for?
What can I create with it?
How is this different from tools like Figma?
How is this different from vibe coding tools?
Can I use Miro Prototyping without enabling Miro AI?
Is my data used to train your AI models?
How does pricing work?
Is Miro Prototyping available for Enterprise plans?
Limited Availability
Collaborative AI prototyping
Turn messy ideas and structured research into professional, editable prototypes in minutes. Explore more directions, iterate faster, and align on better solutions before moving to design tools or code.
More than 90M users and 250,000 companies are collaborating in the Innovation Workspace
Why choose Miro for prototyping?
Explore more ideas and refine them easily
Align on direction to make quicker team decisions
Engage customers with visuals for faster buy-in
How it works
Turn what’s already on your canvas into prototypes in minutes. Miro Prototyping is built for fast, flexible collaboration—whether you’re exploring features or running a workshop.
Create with AI
Generate multi-screen prototypes from sticky notes, screenshots, diagrams, or prompts using AI.

Start from a screenshot
Upload screenshots of apps or sites and turn them into mockups—no design files needed.

AI powered editing
Refine and remix with AI. Toggle between variations, tweak layouts, and land on the version that works best.

Preview and click through
Bring flows to life with clickable prototypes and guided hotspots—perfect for sharing, testing, and fast feedback.

Style with brand assets
Upload a brand asset or screenshot to apply your colors—making prototypes feel more real with less effort.

Edit with drag-and-drop
Customize screens using editable components built for product flows.

Loved by product teams
Try the most popular templates tailored for your team
You’ll never need to start from scratch. Tap into Miro’s huge library of customizable templates, built for your everyday workflows.

Create product prototypes, conduct usability testing, and gather stakeholder feedback.
21000b3c-2496-4e73-bc94-b59192206517

Visualize and iterate website designs using the latest AI capabilities for improved prototyping. Start off with our website prototype template.
95e82821-80c4-40d9-a78e-3c6eb1e720bc

Streamline the creation and refinement of mobile app designs with the mobile app prototype template. Have a structured yet flexible framework that allows teams to quickly sketch, iterate, and perfect their app concepts.
78622b37-d691-4abd-a069-fbe4f3bade83

Map out your website elements, bring your vision to life, and create a better user experience.
bd2d2960-f2dd-4ca8-84a2-32d765faf126

Create the best version of your website or app prototype and get feedback early on.
3251bfb5-7a86-4987-aa30-75d35272caa8
Need help getting started?
Access free courses to ace the canvas in no time, browse through our blog, get quick answers from our Help Center, and more.
FAQs
What is Miro AI Prototyping?
Who is Miro Prototyping for?
What can I create with it?
How is this different from tools like Figma?
How is this different from vibe coding tools?
Can I use Miro Prototyping without enabling Miro AI?
Is my data used to train your AI models?
How does pricing work?
Is Miro Prototyping available for Enterprise plans?
Limited Availability
Collaborative AI prototyping
Turn messy ideas and structured research into professional, editable prototypes in minutes. Explore more directions, iterate faster, and align on better solutions before moving to design tools or code.
More than 90M users and 250,000 companies are collaborating in the Innovation Workspace
Why choose Miro for prototyping?
Explore more ideas and refine them easily
Align on direction to make quicker team decisions
Engage customers with visuals for faster buy-in
How it works
Turn what’s already on your canvas into prototypes in minutes. Miro Prototyping is built for fast, flexible collaboration—whether you’re exploring features or running a workshop.
Create with AI
Generate multi-screen prototypes from sticky notes, screenshots, diagrams, or prompts using AI.

Start from a screenshot
Upload screenshots of apps or sites and turn them into mockups—no design files needed.

AI powered editing
Refine and remix with AI. Toggle between variations, tweak layouts, and land on the version that works best.

Preview and click through
Bring flows to life with clickable prototypes and guided hotspots—perfect for sharing, testing, and fast feedback.

Style with brand assets
Upload a brand asset or screenshot to apply your colors—making prototypes feel more real with less effort.

Edit with drag-and-drop
Customize screens using editable components built for product flows.

Loved by product teams
Try the most popular templates tailored for your team
You’ll never need to start from scratch. Tap into Miro’s huge library of customizable templates, built for your everyday workflows.

Create product prototypes, conduct usability testing, and gather stakeholder feedback.
21000b3c-2496-4e73-bc94-b59192206517

Visualize and iterate website designs using the latest AI capabilities for improved prototyping. Start off with our website prototype template.
95e82821-80c4-40d9-a78e-3c6eb1e720bc

Streamline the creation and refinement of mobile app designs with the mobile app prototype template. Have a structured yet flexible framework that allows teams to quickly sketch, iterate, and perfect their app concepts.
78622b37-d691-4abd-a069-fbe4f3bade83

Map out your website elements, bring your vision to life, and create a better user experience.
bd2d2960-f2dd-4ca8-84a2-32d765faf126

Create the best version of your website or app prototype and get feedback early on.
3251bfb5-7a86-4987-aa30-75d35272caa8
Need help getting started?
Access free courses to ace the canvas in no time, browse through our blog, get quick answers from our Help Center, and more.
FAQs
What is Miro AI Prototyping?
Who is Miro Prototyping for?
What can I create with it?
How is this different from tools like Figma?
How is this different from vibe coding tools?
Can I use Miro Prototyping without enabling Miro AI?
Is my data used to train your AI models?
How does pricing work?
Is Miro Prototyping available for Enterprise plans?
Limited Availability
Collaborative AI prototyping
Turn messy ideas and structured research into professional, editable prototypes in minutes. Explore more directions, iterate faster, and align on better solutions before moving to design tools or code.
More than 90M users and 250,000 companies are collaborating in the Innovation Workspace
Why choose Miro for prototyping?
Explore more ideas and refine them easily
Align on direction to make quicker team decisions
Engage customers with visuals for faster buy-in
How it works
Turn what’s already on your canvas into prototypes in minutes. Miro Prototyping is built for fast, flexible collaboration—whether you’re exploring features or running a workshop.
Create with AI
Generate multi-screen prototypes from sticky notes, screenshots, diagrams, or prompts using AI.


Start from a screenshot
Upload screenshots of apps or sites and turn them into mockups—no design files needed.
AI powered editing
Refine and remix with AI. Toggle between variations, tweak layouts, and land on the version that works best.

Preview and click through
Bring flows to life with clickable prototypes and guided hotspots—perfect for sharing, testing, and fast feedback.

Style with brand assets
Upload a brand asset or screenshot to apply your colors—making prototypes feel more real with less effort.

Edit with drag-and-drop
Customize screens using editable components built for product flows.

Loved by product teams
Try the most popular templates tailored for your team
You’ll never need to start from scratch. Tap into Miro’s huge library of customizable templates, built for your everyday workflows.

Create product prototypes, conduct usability testing, and gather stakeholder feedback.
21000b3c-2496-4e73-bc94-b59192206517

Visualize and iterate website designs using the latest AI capabilities for improved prototyping. Start off with our website prototype template.
95e82821-80c4-40d9-a78e-3c6eb1e720bc

Streamline the creation and refinement of mobile app designs with the mobile app prototype template. Have a structured yet flexible framework that allows teams to quickly sketch, iterate, and perfect their app concepts.
78622b37-d691-4abd-a069-fbe4f3bade83

Map out your website elements, bring your vision to life, and create a better user experience.
bd2d2960-f2dd-4ca8-84a2-32d765faf126

Create the best version of your website or app prototype and get feedback early on.
3251bfb5-7a86-4987-aa30-75d35272caa8
Need help getting started?
Access free courses to ace the canvas in no time, browse through our blog, get quick answers from our Help Center, and more.
FAQs
What is Miro AI Prototyping?
Who is Miro Prototyping for?
What can I create with it?
How is this different from tools like Figma?
How is this different from vibe coding tools?
Can I use Miro Prototyping without enabling Miro AI?
Is my data used to train your AI models?
How does pricing work?
Is Miro Prototyping available for Enterprise plans?
Product
Solutions
Resources
Company
Plans and Pricing
Product
Solutions
Resources
Company
Plans and Pricing
Product
Solutions
Resources
Company
Plans and Pricing
Product
Solutions
Resources
Company
Plans and Pricing











